How To Prevent Toenail Fungus
No one wants to experience toenail fungus (also called onychomycosis). However, it is relatively...
Fungal spores are tenacious and long-lived, as anyone who’s done battle with them will tell you. Spores persist on clothing and shoes, bedding, rugs, and furniture wherever dead skin cells are present. Toenail fungus, called onychomycosis, lurks in shoes and boots where moisture is easily trapped, and fungal spores can remain alive and active from 12 to 20 months.
Superficial fungal infections, particularly fungal nail infections, take anywhere from a few days to a few months to heal, and deep tissue infection may require treatment for up to two years. Cellulitis may develop when a toenail fungus infection spreads beyond the nail, causes cracks in the skin, and allows bacteria can get in. If the cellulitis is severe, the infection may enter the bloodstream – with dangerous, even deadly, results. Dermatophytes, a pathenogenic fungus, can also arise on toenails and fingernails, mucous membranes, hair, and skin and it requires thorough and aggressive treatment.
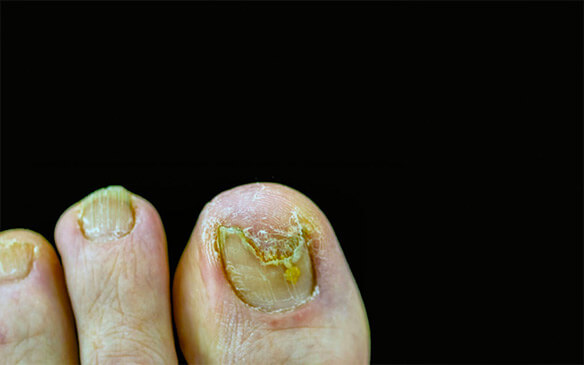
Another common fungus fond of the same environment is athlete’s foot, or tinea pedis. Unlike onychomycosis, this fungal infection thrives also in a dry environment, so is common in summer months among sandal and flip-flop wearers. Athlete’s foot manifests in intense itching; cracked, blistered or peeling skin; and redness and scaling in dry, flaky areas. If you don’t wear socks, dead skin cells may rub off your feet onto your shoes, creating a surprisingly efficient breeding ground for fungi.
Tinea pedis and onychomycosis fungi will remain active on dead skin cells and wait inside your shoes until the next time you slip them on. A dry environment may be less friendly to fungi than a moist environment, but wherever fungi cells are allowed to thrive, the scene is set for infection by toenail fungus spores and athlete’s foot.
If your feet tend to be very sweaty and if you detect a foul odor from your shoes, it’s probably a good time to seek professional attention. See your family doctor to begin treatment. In some cases, your doctor may immediately refer you to a dermatology specialist or to a DPM – a podiatrist – to correctly test and diagnose the fungal infection, determine its severity, and recommend the most effective treatment regimen to defeat it.
Effective options exist and your medical professional will know which anti-fungal tablet, cream, spray, or liquid will work best on your infection. Lamasil, Jublia, and Sporanox are among the most widely prescribed, depending on a person’s age and the type and severity of the fungal infection. All these treatment regimens work by encouraging new nail growth free of infection. Because the infected nail can be replaced only by the slow nail growth process, you must take these medications for six to 12 weeks, or longer.
Adopt good foot hygiene habits
There are sensible precautions you can take to head off toenail fungal infection, foot fungus and athlete’s foot in the first place — or to prevent reinfection after successful treatment.
* Don’t wear anyone else’s socks or put on their shoes. Keep in mind that if they have a toenail fungal infection, it will then likely become yours.
* Wash and thoroughly dry your feet daily, especially between the toes where moisture collects and where fungal spores may find a home.
* And those little boxes of disposable socks at the shoe store? Always put them on before you try on any pair of shoes.
* Wear flip-flops or shower shoes in locker rooms, around swimming pools, and in gym showers.
* Regularly use shoe sanitizer and anti-fungal spray, as directed, to help guard against athlete’s foot and toenail fungus infection or reinfection.
* Sprinkle antifungal powder daily on your feet and in your socks and shoes, especially if you have sweaty feet.
* After your toenail fungus has been defeated use an antifungal cream or antifungal foot powder daily to help maintain good foot health. Continue for at least one or two weeks after treatment.
* About those pedicures: If you already have toenail fungus, a pedicure won’t cause you any harm or make a fungal infection any worse, but be sure to alert the salon staff ahead of time so they’ll know to sterilize tools and equipment used for your pedicure. They may ask you to bring your own nail grooming kit, including nail clippers, trimmer, and file. Giving up nail polish is a wise idea, since lacquers will seal any fungal nail infection into the nail bed and impede good treatment results.
While over-the-counter preventives and treatment options cannot replace medical intervention to address an active fungal spore infection, there are some common household products, such as vinegar, that have antifungal properties and may be useful in maintaining general foot hygiene and surface toenail health. Other home remedies include alcohol rub hand sanitizers kill most surface bacteria and fungi; baking soda (sodium bicarbonate) is an antifungal agent and can be added to a foot soak; hydrogen peroxide kills fungus and bacteria that could cause an infection and may be applied to the surface of the foot; soaking your feel in a tablespoon of bleach in half a gallon of water will help kill fungus; and tea tree oil is a very popular antifungal agent you may mix with herbs and a carrier oil and apply with a swab to infected areas several times a day. Keep in mind that these remedies are not fully proven and may be insufficient when dealing with a toenail fungus infection.
Rubbing alcohol and disinfectants, such as Lysol, will kill fungus on surfaces and in the laundry. If your shoes can be laundered in very hot water, that will kill fungal spores (but alas, maybe your shoes, too). And foot powder containing cornstarch and zinc oxide sprinkled into socks and shoes will keep feet dry and help control athlete’s foot.
Overall, Clear + Restore is often recommended by doctors to be used by patients along with their prescription anti-fungal medication. This will ensure efficacious results will be seen quicker.
Try Clear + Restore to help restore fingernails and fix toenail fungus symptoms today!
Find out more about Toenail Fungus Treatment & Fungus prevention tips here
Is it safe to spray Lysol on a toe nail that has fungal infection rather than using something like Ciclodan?